Mini Review - Interventional Cardiology (2023)
Malpractice in cardiology: A review of literature
- Corresponding Author:
- Mónica Hernández Herrero
Collaborating researcher, Health Law and Bioethics Group, IDIVAL-University of Cantabria, Loredo-Cantabria, Spain,
E-mail: gasiosa@hotmail.com
Received date: 26-Jun-2023, Manuscript No. FMIC-23-103788; Editor assigned: 28-Jun-2023, PreQC No. FMIC-23-103788 (PQ); Reviewed date: 12-Jul-2023, QC No. FMIC-23-103788; Revised date: 19-Jul-2023, Manuscript No. FMIC-23-103788 (R); Published date: 28-Jul-2023, DOI: 10.37532/1755- 5310.2023.15(S18).447
Abstract
Medical liability is a major concern for health care professionals and the entire health care system. Health care activity carries a risk of malpractice lawsuits, but this risk is overestimated. This results in physicians trying to defend themselves from lawsuits by practicing defensive medicine, which is very detrimental to the entire system. A study of medical liability lawsuits shows that, even if a lawsuit is filed, it is decided in favor of the defendant in most cases. Medical specialty is one of the factors affecting the likelihood of a lawsuit. Although cardiology is considered a low-risk specialty, we believe that the relevance of cardiovascular diseases and their repercussions on people’s health is more than enough reason to delve into the current state of malpractice in cardiology. The study of medical liability is not widespread. However, we maintain that it is fundamental for a better understanding of medical–legal aspects among professionals. As a fundamental strategy we propose to further investigation into the analysis of rulings related to medical liability claims. In this way, risk estimation may more closely resemble reality and, as a consequence, we will be able to avoid the practice of defensive medicine.
Keywords
Cardiovascular disease • Insomnia • Depression
Introduction
Clinical practice carries a number of risks, including the risk of a medical liability lawsuit. Physicians overestimate the risk of a malpractice because of several reasons [1,2]. Doctors perform countless medical acts on a daily basis. Nevertheless, if they breach the lex artis ad hoc by Tomillo [3], (standard of care), may involve them being immersed in a lawsuit. Lex artis is the legal criterion to determine the correctness of medical practice and include the consent informed. In the field of medical liability, a series of factors can help us to understand the interest of the study of malpractice claims. Firstly, the doctor–patient relationship has been changing over the last few decades, particularly due to the strengthening of patient autonomy. This factor has been influenced by improved access to information and, above all, by advances in patients’ rights through the delimitation of medical liability. These limits have been introduced by the juridification of medical acts [4], or in other words, the penetration of legal rules on medical acts. This means that patients can be compensated for a breach of the duty of care. Secondly, the costs of medical care are increasing. For example, in the US between 1970 and 2019, total health care spending increased from 6.7% of the Gross Domestic Product (GDP) to 17.7% of the GDP. Comparing these data with the average of the Organization for Economic Cooperation and Development (OECD) countries, which is 8.8%, shows that spending is more than double in the US [5]. The factors contributing to the increase in health spending are numerous, including demographic factors and advances in new technologies and drugs. Within these factors, spending on medical liability accounts for a non-negligible percentage of total spending. The costs associated with malpractice are increasing in some countries, such as the UK, The total annual cost of NHS litigation stood at £3.6 b (2018/2019), which is over three times greater than in 2008/2009 (£970 m); this increase is posing a real challenge to the sustainability of the health care system [6]. Third, one of the direct consequences of the increase in medical liability claims is the use of defensive medicine. Defensive practices are the performance of unnecessary diagnostic tests and treatments (positive defensive medicine) or, alternatively, the rejection of high-risk patients (negative defensive medicine) [7]. Defensive medicine is one of the most frequent causes of overutilization, and its contribution to health care spending is not negligible, estimated in the US at 2.4% of total spending [8]. Fourth, medical errors are directly related to the three factors discussed above. We should point out that medical errors have been known since antiquity, and despite the advances made in recent decades in relation to patient safety, medical errors continue to be an incalculable source of harm to patients. For example, it has been estimated that medical errors could be the third leading cause of death in the US [9].
Literature Review
However, we must emphasize that not every error means malpractice, but that a series of requirements must be met to be considered negligence. Medical malpractice is a deficient practice, that is, is the failure to take reasonable care to avoid causing injury to another person (breach of the lex artis). Finally, studies have shown that medical malpractice litigation negatively affects professionals’ health. Specifically, it could produce psychological damage, for example: Irritability, low mood, insomnia, depression [10,11].
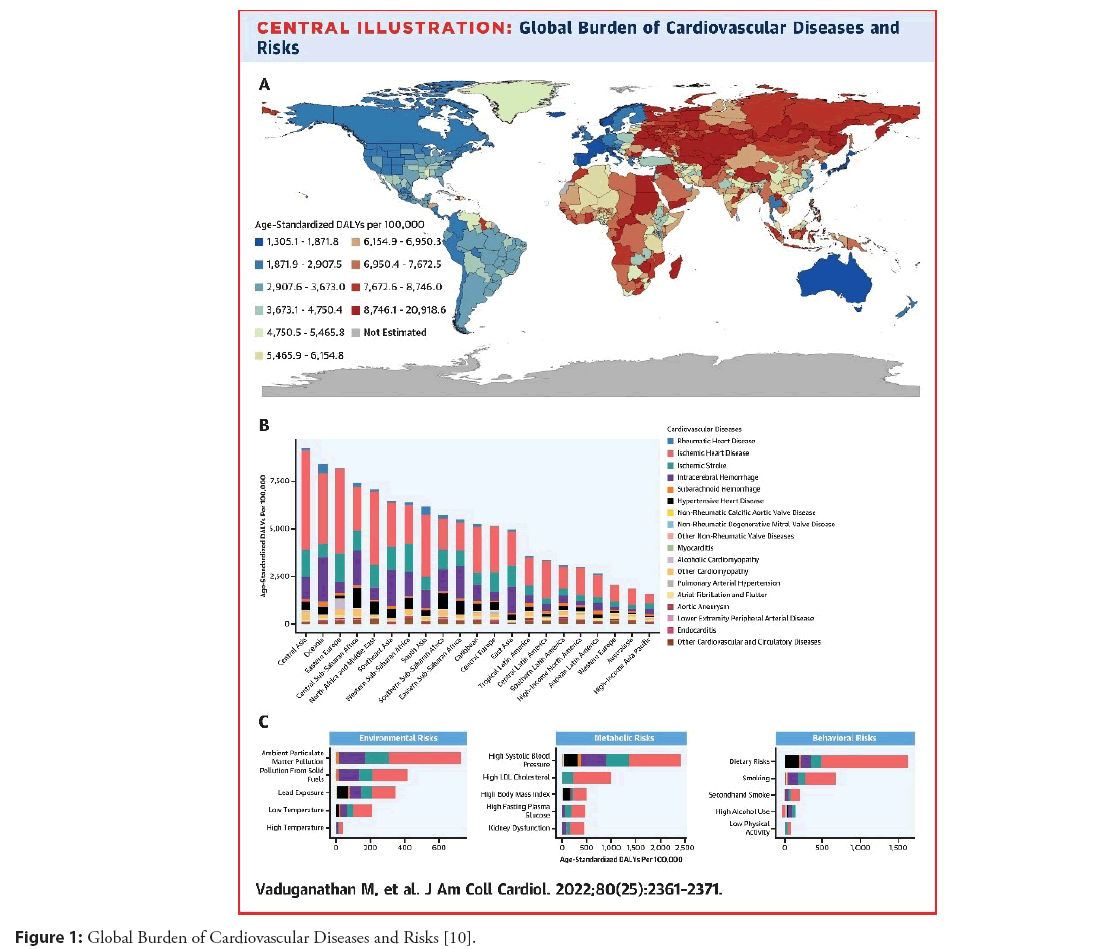
Cardiovascular health is an indisputable challenge for health care systems. Cardiovascular diseases are the leading cause of death in the world, with a significant loss of quality of life and very high associated costs. For all these reasons, cardiology specialists’ role in health care is particularly relevant (Figure 1) [12]. Furthermore, cardiology is a specialty with higher rates of malpractice suits than average. That why, a better understanding of the characteristics of these liability claims can help cardiologists mitigate the risk of malpractice and consequently could improve patient safety.
Figure 1: Global Burden of Cardiovascular Diseases and Risks [10].
Discussion
Determining the risk of a medical liability claim is complex. The authors state that this risk affects three circumstances: a) the specialty, b) the judgment in favor of the plaintiff, and c) the amount of such payment [13].
Specialty
Advances in the field of cardiology are indisputable. A series of techniques have been developed from the 20th to 21st century, among which the following stand out: Electrocardiography, preventive cardiology, the creation of coronary units, echocardiography, thrombolytic therapy, coronary catheterization and angiography, surgery, automatic implantable cardiac defibrillators, coronary angioplasty, and nuclear magnetic resonance for the non-invasive quantification of cardiac function [14,15].
Despite all the advances, physicians involved in cardiovascular health are not infallible and can make mistakes at any stage of health care [16]. In addition, cardiologists may become involved in medical liability lawsuits. Such a possibility is a major concern for them, even conditioning about 50% of their decisions [17]. The cardiology specialty is not considered high risk, although claims frequency data show it to be 8.6% in the US, above the average for physicians in general, 7.4% [13]. In Italy, cardiology is estimated to be involved in 6.7% of cases [18]. In Spain, a study of liability lawsuits in the public sector showed that cardiologists were involved in 2.2% [19], ranking 14th out of all the specialties analyzed [20]. As a consequence of the fear of a lawsuit, defensive medicine arises, the study of which is very complex. The prevalence of defensive medicine varies throughout the world, from 93% in the US [21], to 60% in Italy [22]. In particular, defensive medicine in cardiology has hardly been investigated. In a study conducted in the US, defensive medicine was observed to be the factor most associated with cardiologists’ variability in assessing and treating [23].
The failure of claims
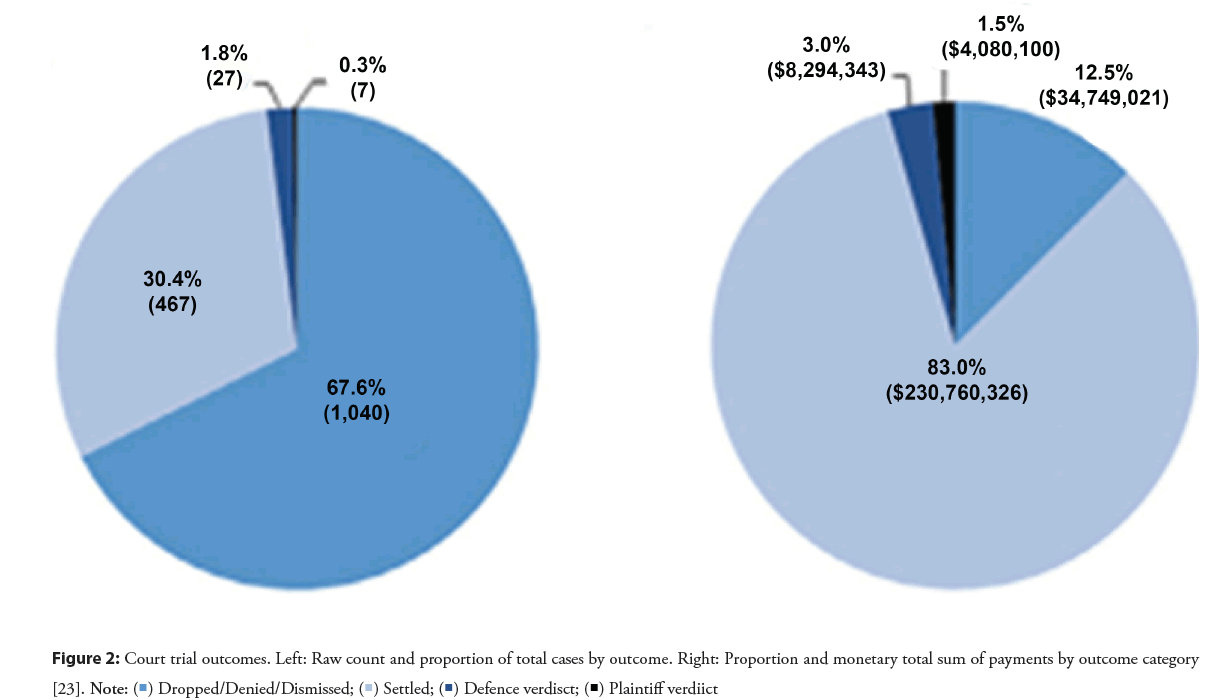
Internationally, scientific evidence shows that most claims are decided in favor of the defendant. A study in the US between 2010 and 2015 found that more than half of the cases (56.6%) were decided in favor of the defendant [24]. Another US study that analyzed 1538 claims between 2006 and 2015 found that more than two-thirds of the cases were decided in favor of the defendant, dismissed, or denied (Figure 2) [25].
Figure 2: Court trial outcomes. Left: Raw count and proportion of total cases by outcome. Right: Proportion and monetary total sum of payments by outcome category [23]. 
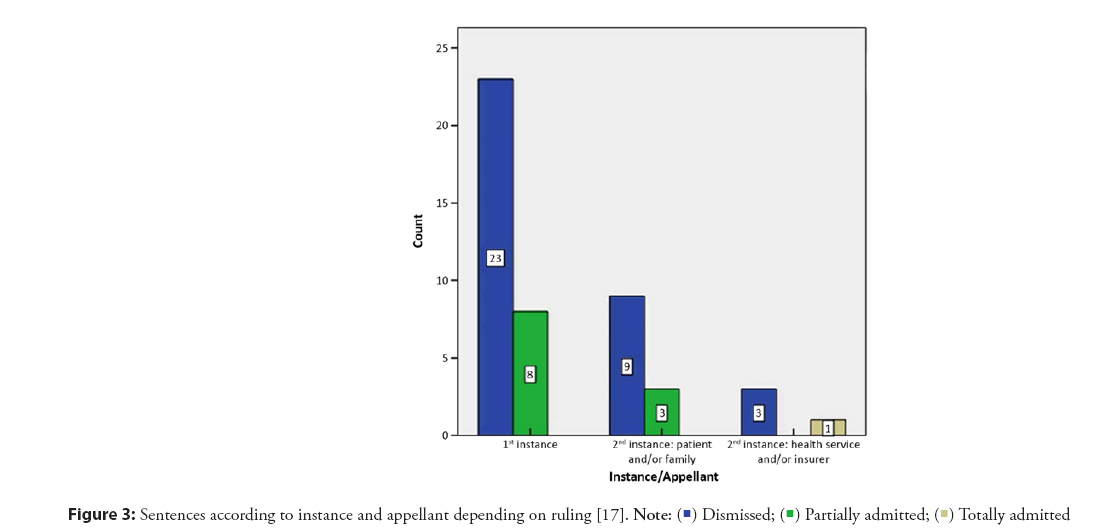
In a study in Spain, claims in the public setting involving cardiology specialists were decided in favor of the administration in two-thirds of the cases analyzed (Figure 3) [18].
Figure 3: Sentences according to instance and appellant depending on ruling [17]. 
The findings in the international literature show that most judgments are unfavorable to the plaintiff. This reinforces our idea that the fear of lawsuits is exaggerated-even if they do occur, most outcomes favor the defendant. This result is very important; physicians must be aware of it to avoid or reduce unjustified defensive practices.
Compensation amounts
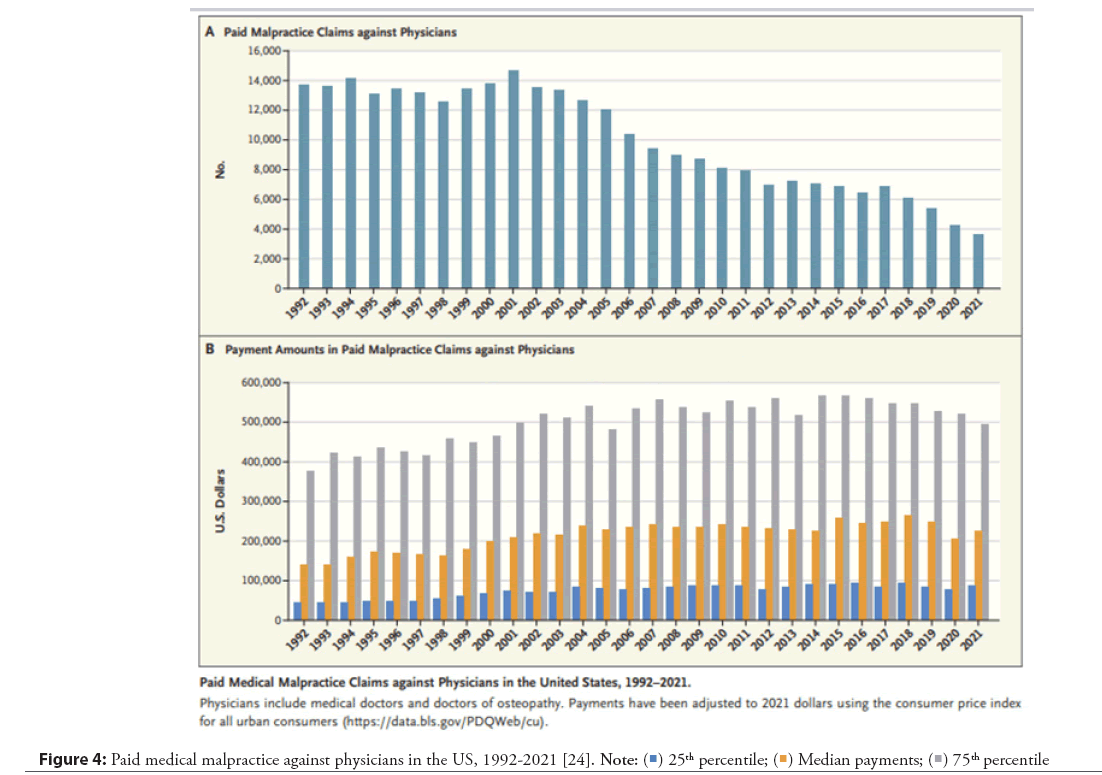
First, we would like to point out that it is very difficult to make comparisons between countries in terms of payment amounts, due to the socioeconomic differences between countries. However, in general, payments in different specialties have been increasing over the last few years, although there are some exceptions. The current malpractice scenario in the US is different from that in other countries. First, only 1 in 20 claims end in a trial, as many are resolved through out-of-court dispute resolution mechanisms, and others are dismissed. Data from the National Practitioner Data Bank (NPDB) indicate that paid claims against physicians have declined by 75% over the past 20 years for a variety of reasons, and the median payout has doubled (Figure 4) [26].
Figure 4: Paid medical malpractice against physicians in the US, 1992-2021 [24]. 
According to a National Health Service (NHS) report, compensation to claimants has increased by 10.3% [27]. In Spain, median compensation amounts remained stable in the public sector between, 2008 and 2020, [18]. Secondly, we found very few studies that specifically refer to compensation in the field of cardiology. In a study in the US, cardiologists had a mean and median compensation amount above those for all specialties, although they did not have the highest amounts [28]. A study in Catalonia that analyzed claims and their awarded amounts showed a median of 153,249 euros in cardiology [29]. Another study of claims in the public health system found a median of 15,000 euros for cardiology, below the median compensation for other specialties [21].
Conclusion
The studies reviewed show that cardiology is generally considered a low-risk specialty. Given the favorable results for defendants in the event of a lawsuit, it is of great interest to raise awareness of these medical-legal aspects, which in turn are little known and studied by professionals. Due to the worldwide increase in the use of defensive medicine and its enormous negative consequences for the entire health system, we believe that these data can help to better frame the real risk of lawsuits and reduce defensive practices. Besides, there are another strategies that could be successful:
• Improve the communication between doctors and patients increasing time to attend in consultations, promote bioethics.
• Structured training essential in medico-legal aspects from undergraduate medical students to experienced doctors for the practice of the profession.
• Introduce the extrajudicial mechanisms conflicts to avoid expensive lawsuits.
References
- Dick JK, Gallagher TH, Brenner RJ et al. Predictors of radiologists’ perceived risk of malpractice lawsuits in breast imaging. AJR Am J Roentgenol. 192(2):327-333 (2009).
- Carrier ER, Reschovsky JD, Mello MM et al. Physicians’ fears of malpractice lawsuits are not assuaged by tort reforms. Heatlh Aff. 29(9):1585-1592 (2010).
- Tomillo Urbina J. omillo Urbina J. New patient rights from their legal status as a consumer. Law and Health. 19:46 (2010).
- Cayón de las Cuevas J. The provision of health services as a legal consumer relationship. Navarre. Thomson-Reuters. (2017).
- Predictors of radiologists’ perceived risk of malpractice lawsuits in breast imaging
- Lane J, Bhome R, Somani B, et al. National trends and costo f litigation in UK National Heatlh Servicie (NHS): A specialty-specific análisis from the past decade. Scottish Medical Journal. 66(4):168-174 (2021).
- Tancredi LR, Barondess AJ. The problem of defensive medicine. Science. 200 (4344):879-882 (1978).
- Mello MM, Chandra A, Gawane AA, et al. National costs of the liability system. Health Aff. 29:1570 (2010).
- Makary MA, Daniel M. Medical error-the third leading cause of death in the US. BMJ. 353: i2139 (2016).
- Vizcaíno Rakosnik BA, Martín Fumadó C, Arimany Manso J, et al. The impact of malpractice claims on physicians´ well being and practice. J Patient Saf. 18(1):46-51 (2022).
- Robertson JJ, Long B. Suffering in silence: Medical error and its impact on health care providers. J Emerg Med. 54(4):402-409 (2018).
- Vaduganathan M, Mensah GA, Turco J, et al. The global burden of cardiovascular diseases and risk: A compass for future health. J Am Coll Cardiol. 80 (25): 2361-2371 (2022).
- Jena AB, Seabury S, Lakdawalla D, et al. Malpractice risk according to physician specialty. N Engl J Med. 365(7):629-636 (2011).
- Metha NJ, Khan IA. Cardiology`s 10 Greatest Discoveries of the 20th century. Tex Heart Inst J. 29 (3):164-171 (2002).
- Glosh SK, Priya A, Narayan RK, et al. Evolution of the fabrics in cardiovascular science: An enduring process of refinement. Ann Cardiool Angeiol (Paris). 70 (4): 220-230 (2020).
- Ohta Y, Miki I, Kimura T, et al. Epidemiology of adverse events and medical errors in the care of cardiology patients. J Patient Saf. 15(3):251-256 (2019).
- Badri M, Abdelbaky A, Yan GX, et al. The impact of medical malpractice litigation on cardiovascular practice in the US and China. Int J Cardiol. 11(1):48-50 (2014).
- Toraldo DM, Vergari U, Toraldo M, et al. Medical malpractice, defensive medicine and role of the "media" in Italy. Multidiscip Respir Med. 10(1):12 (2015).
- Hernández Herrero M, Cayón de las Cuevas J. Litigation in cardiology and cardiovascular surgery: A cross-sectional observational study of liability in the Spanish public healthcare system. Span J Leg Med. 48:136-137 (2022).
- Hernández Herrero M, Defensive medicine and judicialization: X-ray of litigation in public health. (2023).
- Studdert DM, Mello MM, Sage WM, et al. Defensive medicine among high-risk specialist physicians in a volatile malpractice environment. JAMA. 293:2609-2617 (2005).
- Panella M, Rinaldi C, Leigheb F, et al. Prevalence and costs of defensive medicine: A national survey of Italian physicians. J Health Serv Res Policy. 22:211-217 (2017).
- Lucas FL, Sirovich BE, Gallagher PM, et al. Variation in cardiologists' propensity to test and treat: Is it associated with regional variation in utilization? Circ Cardiovasc Qual Outcomes. 3(3): 253-260 (2010).
- Patel R, Rynecki N, Eidelman E, et al. A qualitative analysis of malpractice litigation in cardiology using case summaries through a national legal database analysis. Cureus. 11(7): e5259 (2019).
- Wang F, Sandeep K K. Medical malpractice claims within cardiology from 2006 to 2015. Am J Cardiol. 123(1): 164-168 (2019).
- Studdert, David M, Mark A Hall. Medical malpractice law-doctrine and dynamics. N Engl J Med. 387(17): 1536 (2022).
- CrossRef
- Jena AB, Seabury S, Lakdawalla D, et al. Malpractice risk according to physician specialty. N Engl J Med. 365(7):629-36 (2011).
- Arimany-Manso J, Gómez-Durán EL, Aubia-Marimon J, et al. Professional liability claims for specialties in a scenario other than the United States. Gac Sanit. 27(1):92-93 (2013).